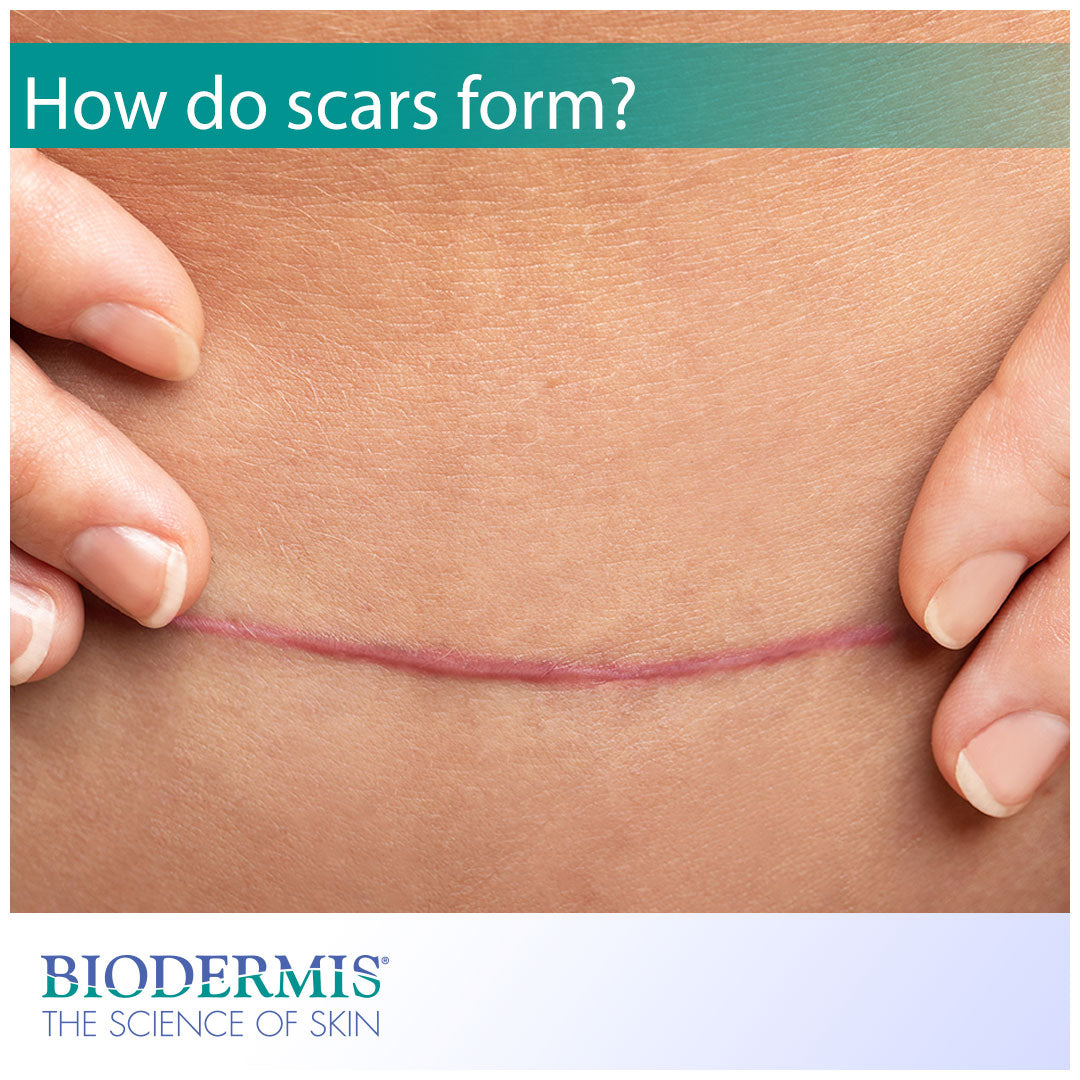
Scar formation
The dermis and epidermis layers of the skin play pertinent roles in scar formation and work to facilitate a natural, biologic process of wound repair. When a person sustains a wound that penetrates the middle layer of the skin—the dermis—the skin repair response begins. Damage to the dermis layer signals fibroblast skin cells to synthesize massive amounts of collagen. The collagen is then sent to the wound site, promoting the growth factor, and rebuilding new skin tissue. The epidermis flaunts the new tissue as a scar, which can appear discolored and raised.
Collagen type I is responsible for giving our skin its elastic, durable nature and supple appearance. When it comes to skin repair and scar formation, collagen plays an integral role in promoting new tissue growth at the wound site. Scar tissue is on average 20 percent weaker than pre-damaged skin; so even though this protein is known to promote strength in our vital organs, it begins to break down as we age or undergo trauma. As we age, our bodies naturally begin to produce less collagen. This is the reason older adults begin to develop fine lines and wrinkles. Other factors that lead to collagen loss or a decrease in collagen production include smoking, drug abuse, and extended exposure to ultraviolet radiation from the sun.
Types of scars
Keloid and hypertrophic scars are cutaneous conditions that sometimes occur as a result of excessive collagen production; these are the scars most people wish to avoid. Keloid scars, also known as keloidal scars, are characterized by lumpy, ropey growths on the skin, often purple or red in color. Keloid scar tissue tends to branch out, covering a larger skin area than the wound itself.
Hypertrophic scars are raised and rigged in appearance, with a red or purple complexion. Though not as severe as keloid scars, hypertrophic scars can still be unappealing and painful. Both scar types can occur as a result of a surgical procedure or injury, in addition to any form of piercing or acne scarring.
Age and genetics influence scar formation
As you get older, skin becomes thinner and wounds take longer to heal. However, old age is also correlated with less scarring. The reasons for this aren’t scientifically clear yet, but it may have to do with a specialized compound secreted in the bloodstream. Along with age, genetics also play a role in scar formation. The American Academy of Dermatology (AAD) states that people of African, Asian, or Hispanic descent are more likely to develop keloid scars than other ethnicities. Furthermore, if you have a family history of keloids, then you will also be at higher risk for developing them.
Scar treatment options
Scars can be treated in a variety of different ways, such as corticosteroid injections, laser therapy, and surgical removal. However, one of the safest and most effective topical solutions is medical-grade silicone gel for scars. Silicone gel is backed by more than 30 years of clinical evidence and is trusted by surgeons and dermatologists around the world. Silicone gel works simply and effectively through the mechanisms of dermal hydration and collagen regulation. Products can be purchased through your physician or online at biodermis.com.
Biodermis is an innovative market leader with 30 years of expertise in the medical silicone industry. Visit Biodermis.com today to explore a complete range of scar management and post-operative care solutions.
Biodermis offers custom tailored referral programs designed to simplify and reduce the cost of your patients' post-op care. Additionally, we offer professional pricing if you opt to retail our products. Give us a call at 800.322.3729, and we will be happy to provide additional details on these programs.