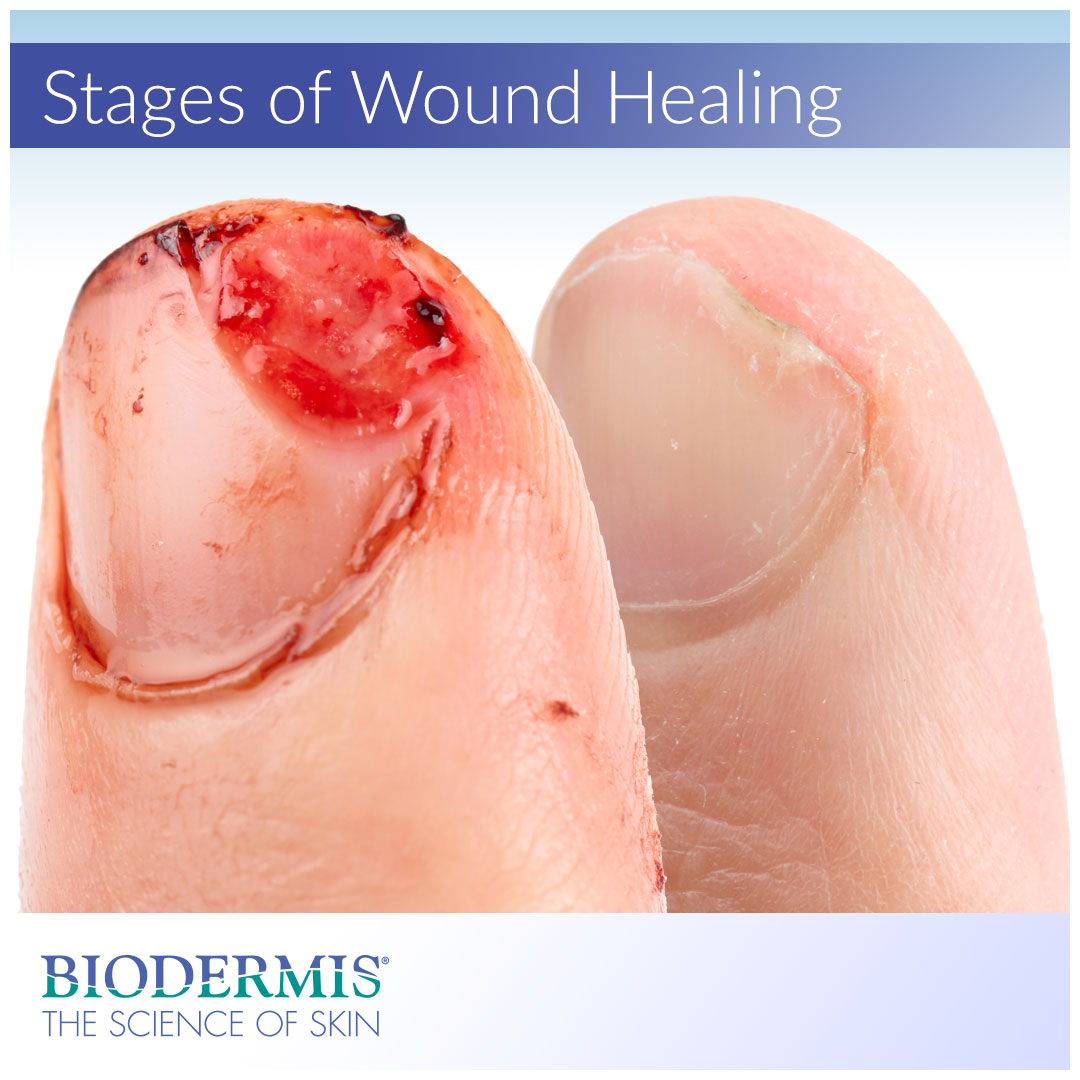
When a person sustains a wound from trauma or injury, an intricate and dynamic wound-healing process is triggered. The phenomenon of wound healing is represented by four distinct stages: hemostasis, inflammation, proliferation, and maturation. Each successive phase is characterized by vital biochemical processes necessary for the well-being of an individual and the regeneration of cellular structures. If a wound is detrimental enough, blood clotting and tissue regeneration will culminate in a scar. Each scar is a tangible reminder of the cascade of events that promote wound healing and tissue repair.
The four phases or wound healing
Traditionally, three phases of wound healing were recognized and defined: inflammation, proliferation, and maturation. These phases may be denoted by different names depending on the author. Some refer to the proliferation stage as fibroblastic or granulation, and the maturation stage as remodeling. Later, authors and doctors determined four stages of wound healing with the addition of the hemostasis phase occurring before inflammation. Some consider hemostasis to be part of the inflammation stage. It’s important to know that the biochemical activities present in one stage may overlap and interplay with others. Therefore, the moment one phase ends and the next begins is difficult to clearly identify.
Hemostasis is the first stage of wound healing that acts as a mechanism of first response to injury. Immediately after a person sustains a wound, blood vessels in the trauma area constrict to slow blood loss in a process known as vasoconstriction. Platelets are then released at the wound site to coagulate with fibrin (fibrous protein). The aggregation of platelets and fibrin forms a thrombus, or blood clot, that seals broken blood vessels and stymies blood loss. This entire process can last for two or more days. Covering a wound with a bandage or gauze can facilitate hemostasis and blood clotting.
Inflammation is a physiological event characterized by blood vessel dilation shortly after hemostasis has been achieved. The primary function of what is known as vasodilation is to stave off infection during the wound healing process. A number of beneficial enzymes and leukocytes (white blood cells) enter the wound area to facilitate inflammation during vasodilation. These beneficial cells and molecules are known as exudates that travel through plasma from local capillaries at the wound site. The physical traits of the inflammatory stage are marked by redness at the wound site, pain, swelling, and heat. This second phase of healing can last for six days or more after the initial onset of the wound. Biochemical activities present during inflammation overlap and interplay with those from hemostasis.

Proliferation is the third stage of wound healing characterized by the formation of granulation tissue through a process known as angiogenesis. Granulation tissue is an extracellular matrix consisting of new connective tissue and blood vessels that replace damaged tissue after trauma. This new tissue is often pink or red in appearance due to inflammatory agents—an indication of normal wound healing. Tissue regeneration in this stage relies on fibroblast activity and collagen (structural protein) production. This entire process can last for two or more weeks after trauma. Adequate levels of moisture and oxygen are necessary for the normal functioning of proliferation in wound healing.
Maturation is the fourth and final stage of wound healing commonly referred to as remodeling. This phase can last for up to two years after the wound has contracted and closed. Collagen production aimed at regaining tensile strength and skin elasticity continues to persist during maturation. Collagen buildup in the granulation tissue leads to the formation of a scar. Wound maturation also exhibits a stabilization of vascularity from the inflammation and proliferation stages. Cells and other molecules prevalent in these previous stages engage in apoptosis, otherwise known as programmed cell annihilation. Scar tissue formed during maturation is on average 20 percent weaker and less elastic than pre-injured skin.
Scar formation and management
In excessive amounts, collagen production and buildup can lead to keloid and hypertrophic scar formations. This happens when fibroblasts and keratinocytes in the skin work overtime to restructure and rebuild damaged tissue. Abnormal scarring can appear raised and discolored, and because scar tissue lacks hair follicles and sweat glands, can feel itchy and painful.

The only clinically-proven topical solutions for the prevention and reduction of abnormal scar formations are silicone gel sheets, silicone ointments, and silicone sticks. Medical-grade silicone works by inducing moisture and regulating collagen production at the scar site to soften and flatten old and new scars. By achieving homeostasis of moisture and oxygen at the scar bed, collagen production scales back to a stabilized level. This helps scar tissue blend in with the surrounding area, regain functionality, and appear more cosmetically acceptable.
Biodermis is an innovative market leader with 30 years of expertise in the medical silicone industry. Visit Biodermis.com today to explore a complete range of scar management and post-operative care solutions.
Biodermis offers custom tailored referral programs designed to simplify and reduce the cost of your patients' post-op care. Additionally, we offer professional pricing if you opt to retail our products. Give us a call at 800.322.3729, and we will be happy to provide additional details on these programs.