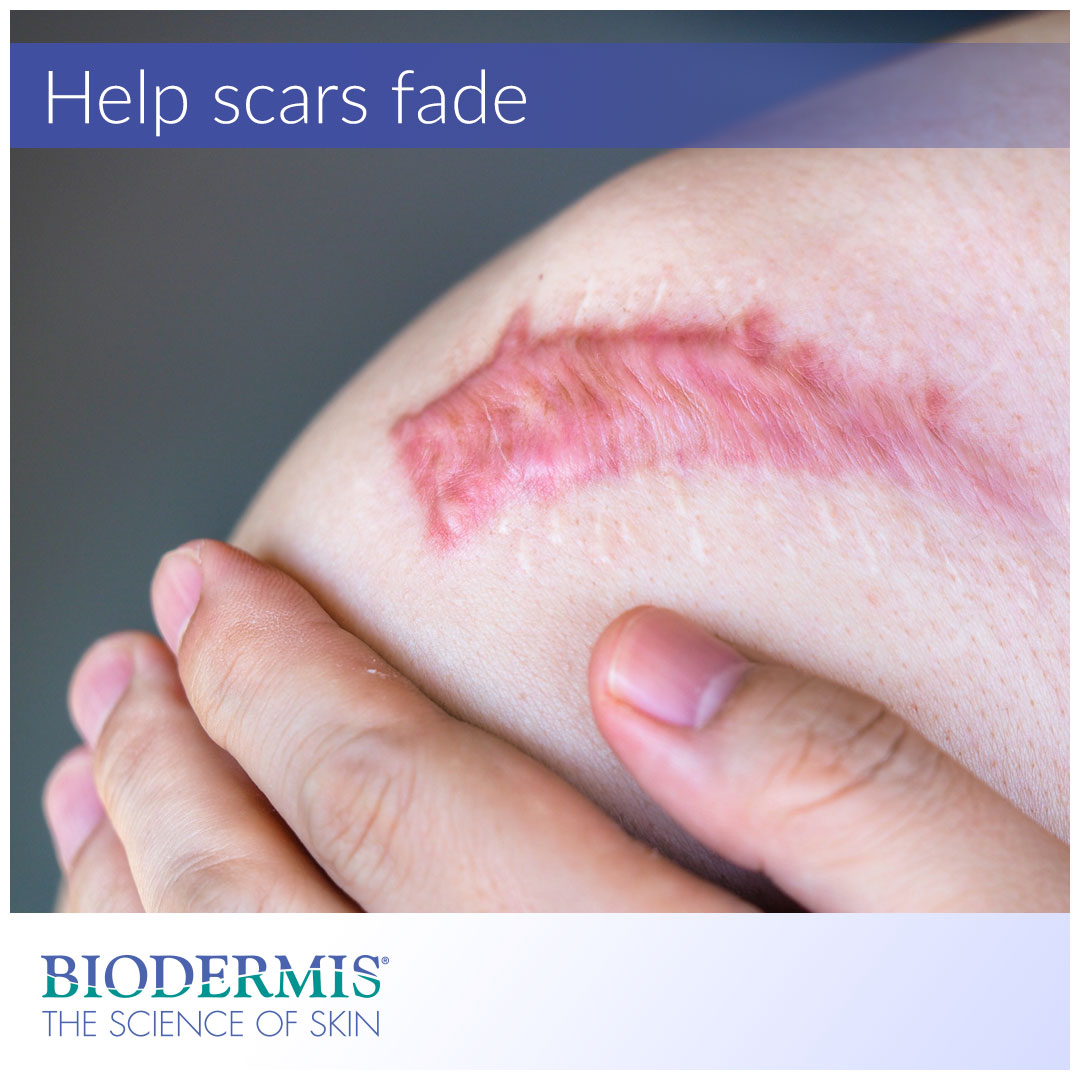
Continue reading to learn more about wound-healing and scar management, and to discover a safe and effective topical solution to flatten and reduce abnormal scar types.
Being mindful of wound healing
The wound healing process is part of a dynamic orchestra of overlapping stages characterized by an interwoven play of biochemical activities. Four stages of wound healing have been identified and defined: hemostasis, inflammation, proliferation, and maturation (remodeling). It’s possible, rather easy in fact, to disrupt any one of these stages, delaying the wound healing process and exacerbating future scar tissue growth. This is one reason we have a healthcare market full of wound care products like bandages, anti-bacterial emollients, and disinfecting sprays. For a speedy recovery, it's important to keep a wound hydrated, protected, and clear of free radicals and bacterial agents. If a healing wound is damaged or becomes infected, the wound healing process will be prolonged and lead to greater scarring down the road. Skin dehydration is another nemesis of wound healing that can be prevented by keeping wounds hydrated and covered while they heal.
Scar formation is part of the last stage of wound healing, also known as maturation or remodeling. In some cases, maturation can last for up to a year or longer after the initial onset of the wound. This means that the skin is still in repair mode, fueling scar tissue with collagen, long after the wound has fully contracted and closed. Collagen, the most common structural protein in the body, is scattered in a disorganized fashion during the proliferation phase. But once the wound is patched up, clay (type III collagen) becomes brick (type I collagen), and the damaged skin begins to resemble its former self. Although the body’s repair mechanisms work wonders, wound-healing isn’t a perfect process. Scar tissue has a tensile strength of about 80% of normal tissue and is bereft of pores, follicles, and sweat glands. If collagen production runs out of control, buildup can lead to raised, discolored scars in the form of keloids and hypertrophic scars.
Scars form when a puncture penetrates the middle layer of the skin (dermis) or deeper. If the wound-repair response is left to do its job without interruption, a normal scar will form and usually fade on its own within a few years. Depending on the extent of the trauma, some scars will take longer to fade than others. Additional factors including genetics, skin type, and how well a wound is treated will determine whether or not a scar fades over time. Populations with darker skin tones are predisposed to developing keloids, whereas hypertrophic scars affect all populations equally. Given all of the elements that affect scar formation, there’s no easy metric to use when predicting when a scar begins to fade.

Medical silicone for scar management
One of the best ways to ensure a wound doesn’t develop into a keloid or hypertrophic scar is to use silicone gel sheeting or silicone scar sticks. Silicone gel technology emerged over 30 years ago as the only proven scar therapy solution for topical use. Medical grade silicone works through two mechanisms of action: skin hydration and collagen regulation. Wounds need an ideal balance of moisture and oxygen, otherwise known as homeostasis, to heal properly. Topical silicone allows the user to retain skin moisture that would otherwise evaporate through transepidermal water loss. This induces hydration at the scar site, which in turn signals fibroblast skin cells to scale back collagen production and reduce collagen buildup. This process helps to flatten and smoothen scars, allowing them to blend in with the surrounding tissue.
Ask your surgeon if silicone gel sheeting is right for you, or explore products online today.
PHYSICIANS AND MEDICAL PROFESSIONALS: REFER OR RESELL?
Biodermis offers custom tailored referral programs designed to simplify and reduce the cost of your patients' post-op care. Additionally, we offer professional pricing if you opt to retail our products. Give us a call at 800.322.3729, and we will be happy to provide additional details on these programs.